Some of my thoughts on the term Muscle Tension which seems to have different meanings for different examiners.
Muscle Tension Dysphonia
The terms “vocal hyperfunction” and “muscle tension dysphonia” have several different meanings depending on the person using them.
To me, muscle tension dysphonia is characterized by the vocal folds typically failing to come completely together because two muscles are pulling in opposite directions simultaneously. The vocal folds have the ability to assume the correct position for a task, but do not. This is most likely a learned behavior.
Examples
- A vocal overdoer (someone who likes to talk) over time may develop vocal nodules. It may take many years for them to enlarge but eventually they protrude enough that when the vocal cords come together, the cords position themselves so that the nodules just barely touch. This leaves the actual vocal folds slightly apart. Perhaps this is because it is easier to phonate with the nodules touching than when they are compressed. Along comes a surgeon and the nodules are removed. During the post-operative checkup the vocal folds assume the same position they did before surgery — slightly apart. There are no nodules holding them apart; they just assume that position as if the nodules were still there. Muscle memory is playing a role. Some muscle is preventing the vocal folds from completely closing, yet they can actually close with the appropriate technique. It is analogous to learning a song on a piano for many years, then trying to play the same song on a toy electric piano with keys that are closer together and have different resistance. Your brain is not used to this change and your fingers go where they think they should go rather than where they need to go. Years of behavior need to be relearned. This is true muscle tension dysphonia. Until that other muscle stops competing with the closing muscles, the voice is still impaired.
- The other common example is a young singer who has developed a breathy style of singing. This is achieved by holding the vocal folds apart. It provides a soft edge to the voice and, if it is the desired style, it can be wonderful. Numerous singers make very good livings with this style. However, if one is striving for a clear, efficient style of singing with a high upper end, this muscle tension can severely impair singing. To a certain extent, the patient can begin to feel the difference by phonating with a very harsh, biting sound and then with a very soft-edged, breathy sound on the same note and comparing the difference.
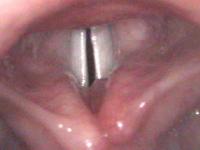
“Hyperfunction” Representing Hypofunction
I think the term muscle tension dysphonia is frequently misused when the examiner notes that the person’s false vocal cords are squeezing together. This may occur either side to side or front to back. It is typically described as the false vocal folds touching during voicing (side to side) or the back of the voice box (the arytenoids) appearing to touch the front (the epiglottis). While this superficially appears to be a hyperfunction, I believe it frequently masks an underlying hypofunction. The hyperfunction is then not the problem — it is a symptom of the problem. The affected person is trying their hardest to produce a good sound and it is extremely effortful. In some cases the false vocal cords are the only possible way to phonate, such as after a substantial portion of the true vocal cord has been removed for cancer. Sometimes the extra squeeze merely brings the true vocal folds closer together or supports a weak true vocal fold.
If one could see below the squeezed false vocal folds (and one can with adequate anesthesia) one would typically find that the true vocal cords are not closing completely or are not staying closed. This may represent a neurologic problem, such as a partial paralysis of one of the several muscles of the voice box. It may represent severe vocal cord bowing — bowing so severe that the vocal folds actually scissor or cross over one another at the back end just to get the middle of the vocal folds close enough together to vibrate. This could represent a lack of tension within the vocal cord, a lack of muscle bulk, or a lack of innervation to one of the muscles.
Patients with this condition will complain of vocal fatigue, poor endurance, and pain in the voice box (typically hot, burning, or achy). This is from excessive use of the neck muscles to support the weakened voice box muscles. The person may have an inability to yell and may have an obligate falsetto — a higher pitched voice than usual.
High pitches are created predominantly by the cricothyroid muscle. This muscle is supplied by the superior laryngeal nerve, a different nerve from the one supplying the rest of the voice box muscles. Because of its separate nerve supply, it often remains healthy even after an injury has impaired the recurrent laryngeal nerve. This muscle basically stretches and lengthens the vocal cords to create a higher pitch, much like tuning up a guitar or violin. If we have a vocal cord that is loose or floppy because the muscle within it is failing, the cricothyroid muscle may pitch in and tighten the vocal cord, increasing the pitch — but at least the person now has a voice. If the person tries to lower the pitch, the voice just gets softer, breathier, and has less volume. Thus the term obligate falsetto — a high pitch just to speak. Therapy directed at relaxing the voice box fails to improve, or even makes the voice less functional.
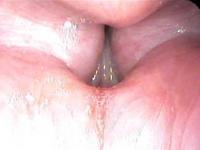
Non-Organic Dysphonia
The third condition that can be lumped under the term “hyperfunction” is a type of non-organic dysphonia. Non-organic dysphonia can present and look like (on video) hyperfunction. In this case, the underlying vocal folds are normal and work well, but an inappropriate behavior has been learned of squeezing tight the upper part of the voice box.
Example
A person may develop laryngitis. The vocal cords become swollen and stiff. To get any voice at all, the person must squeeze extra hard to get the vocal cords together and vibrating. In the process, the false vocal folds are squeezed closer or may even start vibrating to produce a very deep voice. Now a cold should resolve in a reasonable period — perhaps two weeks. However, because of some secondary gain (and this is usually an unconscious gain) the voice problem persists. The types of secondary gain I have seen range from the obvious — “If my hoarseness lasts for a few more days, I’ll be able to collect disability” — to the very subtle. Family or school commitments may have been released because of the illness, or the person is just getting a little extra, much-needed attention from those surrounding them.
This non-organic or learned behavior is very easily and quickly correctable — often during the initial examination — completely restoring a normal voice. Keeping the normal voice may be harder because typically the physician or therapist doesn’t or can’t resolve all the stresses and obligations in a person’s life. The problem may recur unless these other issues are dealt with. This is not “craziness.” This is the way a normal compensatory mechanism becomes the problem itself, and it is the way that our minds work. Recognizing the issues goes a long way to restoring and maintaining vocal health.
Summary
Muscle tension dysphonia or vocal hyperfunction can represent a long-term learned behavior that needs appropriately directed therapy or vocal training to correct. It may represent a compensatory mechanism for an underlying weakness, neurologic paresis, or lack of tension (bowing). This almost never improves with therapy directed at relaxing the “hyperfunction.” Voice building exercises or surgical augmentation to reintroduce bulk and support to the affected vocal fold may be a solution. If the underlying problem is from stiffness, surgery might be directed at softening the vibrating edge of the vocal cord. Thirdly, one form of non-organic dysphonia is a “hyperfunctioning” supraglottis (the false vocal folds). Therapy directed at restoring the normal voice is usually quite successful. In rare cases, deeper probing into the stresses or obligations perpetuating the condition may be helpful.
Therapy directed at relaxing the “hyperfunction” almost never improves the voice when the real problem is an underlying weakness. Voice building — not relaxation — is the solution.
