During an examination, people hate to be embarrassed--they naturally and fairly immediately try to compensate for any hoarseness. It is fortunate that there is redundancy in the vocal system so compensation is usually available to maintain sound production even when there is a problem. However, for the examiner, compensation tends to hide a voice disorder, both audibly as well as visually. Some common instances hidden by compensation include mucosal disorders on the edge of the vocal cord or weakness from neurologic and muscular disorders. Yet the astute examiner eliminates compensation to visually expose a problem.
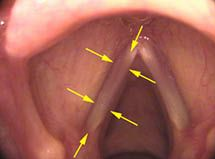
For example, there are two muscles, the ThyroArytenoid (TA) muscle and the CricoThyroid (CT) muscle, which both have the effect of raising pitch. The TA muscle is within the vocal cord and isometrically tightens the vocal cord to raise pitch. In the figure below, arrows outline the generally visible mass of the muscle when viewed from above:
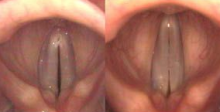
The CT muscle is located on the external surface of the laryngeal cartilages and lengthens the vocal cords to raise the pitch. The figure below shows at left the vocal cords vibrating at a low pitch. At right, the CT muscle has stretched the vocal cords at a high pitch.
If there is decreased neurologic input to one of these muscles, the other muscle compensates at least partially. In the case where the TA muscle is not working on one side, a patient automatically compensates by pulling the CT muscle tighter. This has the effect of raising the speaking pitch when the patient tries to speak with the same volume as before the injury.
When I perform an endoscopic exam on a patient speaking at an unnaturally high pitch, I really want to hear the patient produce a lower and lower pitch. At each lower pitch, compensatory tightness from the CT muscle is progressively removed. As the CT muscle’s contraction is removed, if there is a weak TA muscle, the vocal cord would begin to bow and then flutter in the wind while a healthy TA muscle on the other side would remain tight. Removing compensation amplifies this difference between each side of the larynx and allows improved visualization of this neurologic impairment.
Mucosal disorders – problems with a swelling on the edge of the vocal cord – also involve natural compensation. At higher pitches, the vocal cord is pulled tighter. A mucosal swelling on the edge of a vocal cord would stand out farther and farther with increasing pitch. The further it sticks out, the more likely the swelling is to touch the other vocal cord and stop vibrations. The patient compensates for this “stopping effect” in some instances by increasing the airflow from below to blow the touching swellings apart. In effect, the patient increases their volume to compensate for effects from the vocal swelling sticking out along the edge of the vocal cord.
A singer with a swelling will sing louder and louder as she goes up in pitch to prevent the vocal stoppages. As an examiner, I remove this compensation by asking the patient to make only soft sounds as she goes up in pitch. At low lung pressures, the slightest touch of a swelling on one vocal cord stops or alters the vibrations on both. I remove the volume compensation in order to better hear, visualize and discover the pathology.
Still curious about how we compensate for hoarseness? Read more in "Why is There a Frog in My Throat?"